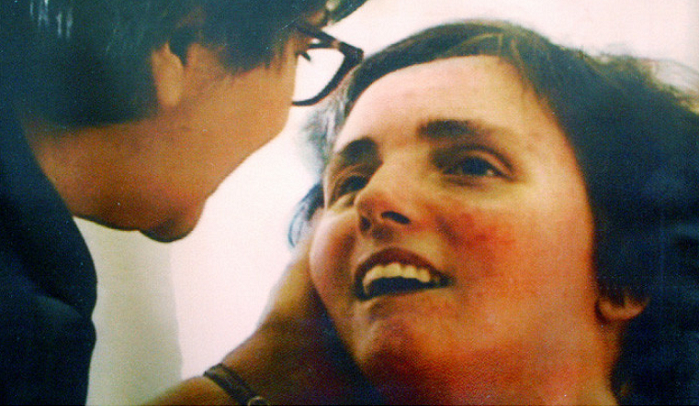
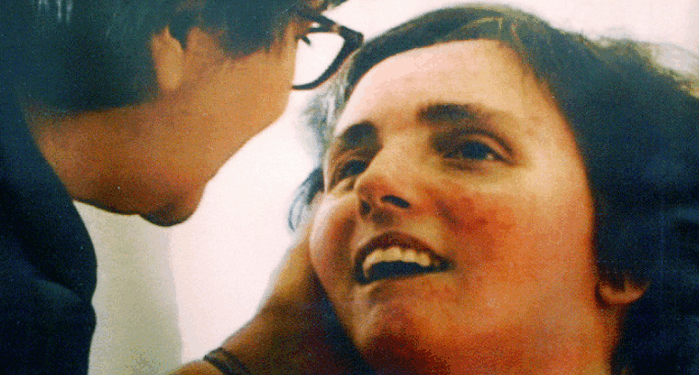Every year on March 31, I honor my sister, Terri Schiavo, and reflect on how our nation treats its most medically vulnerable citizens. Terri’s story is not just a family tragedy; it’s a warning about what happens when the sanctity of life is eroded, and convenience replaces compassion.
Terri was just 26 years old in 1990 when she suddenly collapsed at home with her husband, Michael Schiavo, for reasons that remain unknown. Although Terri sustained a severe brain injury, she was never dying. She had no terminal illness, was not on life-support machines, and was not ‘brain dead.’
With basic care, including a feeding tube necessitated by her swallowing difficulties, Terri could have lived a normal lifespan. However, after just two years, Michael lost interest in caring for his cognitively disabled wife after he began cohabiting with another woman. As Terri’s legal guardian, he subsequently petitioned the courts to remove her food and water.
On March 18, 2005, following an extended legal process lasting more than a decade, Pinellas County Circuit Court Judge George W. Greer authorized the removal of Terri’s feeding tube. After almost two weeks without food or water, Terri died from severe dehydration.
REACH PRO-LIFE PEOPLE WORLDWIDE! Advertise with LifeNews to reach hundreds of thousands of pro-life readers every week. Contact us today.
My family fought desperately to save her, but the courts sided with Michael. Indeed, Terri became the first innocent, disabled American citizen court-ordered to death. Her passing shocked the nation, exposing how quickly society can devalue human life once deemed inconvenient.
In response, my family established a non-profit, the Terri Schiavo Life & Hope Network. Our mission is simple: to stand with families facing similar battles and ensure no one else suffers Terri’s fate. Over the past two decades, the calls we have received have been deeply disturbing. Too many families report that their loved ones, often young people with brain injuries, are written off almost immediately.
Doctors and hospital administrators pressure them to “let go,” to withdraw treatment, or choose comfort care far too soon. Recovery is possible, but only if patients are given time, proper rehabilitation, and basic care. Instead, many are rushed toward death.
The public does not always see the full reality of what brain-injured patients face. Recovery can be slow and unpredictable; some regain speech, movement, or awareness months or even years later. Recent research on brain recovery validates this. Still, today’s system frequently assumes the worst and acts accordingly.
This shift did not happen in isolation. Several powerful cultural and medical influences have converged to make cases like Terri’s routine. Consider the following.
The erosion of tradition has weakened the foundation of medicine. Modern training and ethics often prioritize cost, prognosis, and “quality of life” judgments over the patient’s inherent value, directly influencing treatment decisions.
This crisis has deepened as respect for the sanctity of life has declined. Since the legalization of abortion and the loss of more than 50 million unborn children, our collective belief in the inviolability of every human life has been profoundly diminished. When society accepts ending life in a mother’s womb, it becomes easier to devalue life at any stage, especially when care requires life-preserving resources.
The rise of medical futility policies now empowers facilities to act decisively against the vulnerable, as hospital ethics committees and “medical futility” protocols grant broad power to withhold or withdraw care from those judged to have a “poor prognosis” or no “meaningful hope for recovery.” These policies may appear clinical, but often target the severely brain-injured, disabled, and elderly–the very people most in need of advocates.
The redefinition of basic care has eroded essential protections, as feeding tubes–once widely regarded as part of ordinary humane care–are now classified as “medical treatment,” meaning that they can be denied or withdrawn. This reinterpretation makes nutrition and hydration optional rather than an essential part of basic care and of the universal human rights owed to every person.
The entanglement of brain death and organ donation introduces alarming incentives, as this diagnosis has become intertwined with the urgent demand and billions in annual revenues tied to transplantable organs. Although organ donation can be altruistic, the pressure to declare brain death quickly raises serious ethical concerns.
Out-of-control healthcare costs and rationing pressures exacerbate these challenges, especially for brain-injured patients needing long-term support. Lifetime expenses for severe cases can reach or exceed hundreds of thousands per person, including facility extended care, ongoing rehabilitation, professional caregiving, medications, equipment, home modifications, and lost productivity.
These pressures lead hospitals, insurers, and families to favor quicker decisions to declare care ‘futile,’ withdraw support, or to end treatment, effectively prioritizing efficiency over hope, undermining potential recovery.
The roots of this issue run even deeper into a societal and spiritual drift that has redefined what it means for us to care for one another. The breakdown of the nuclear family has shifted focus from family responsibility to individualism, where the perceived burden often overshadows the sacrificial love needed to care for a brain-injured or elderly loved one.
At the same time, our culture has drifted from the belief that every person bears the image of our Lord and Savior, possessing infinite worth regardless of ability or prognosis.
These influences are not imagined–they directly shape the decisions of doctors, judges, and hospital ethics committees. When life is no longer sacred and faith in Christ Jesus and His teaching to care for “the least of these” is ignored, abandonment becomes the default over hope and duty.
Terri’s death was needless and terribly inhumane. It resulted from choices deep-rooted in a culture that has slowly stopped believing that every life matters. Our work through the Life & Hope Network continues because the battle to care for our medically weak not only persists but is worsening.
On this sad anniversary of Terri’s death, I am left asking whether we are still a nation that respects every life. Have we become so numb that we now measure a person’s worth soley by productivity and convenience?
The choice is ours. Let us protect and defend life, not just in words, but in the policies we support, the care we provide, and the compassion we show. Let Terri remind us to never stop believing in the sacred worth of every life.
LifeNews Note: Bobby Schindler and his family work as patient advocates, establishing the non-profit Terri Schiavo Life & Hope Network in honor of his sister, Terri. Click here to learn more about the Life & Hope Network.