A recent article by Pulitzer Prize–winning journalist Katie Engelhart in The New York Times takes a serious and much-needed look at the diagnosis of persistent vegetative state (PVS).
Titled “Vegetative Patients May Be More Aware Than We Knew,” the piece examines two decades of growing scientific evidence suggesting that nearly half of patients diagnosed as unaware may possess levels of consciousness that standard bedside examinations fail to detect. When you consider the hundreds of thousands of patients who could be affected by this diagnosis, there is reason for alarm.
Engelhart carefully documents the uncertainty surrounding PVS diagnoses, the limitations of current testing methods, and the troubling gap between access to advanced diagnostic tools and the availability of meaningful rehabilitation.
Get the latest pro-life news and information on X (Twitter). Follow @LifeNewsHQ
She highlights the heartbreaking story of Tabitha and Aaron Williams, who are navigating this challenge after Aaron’s brain injury, along with other families facing similar diagnoses and the many medical professionals, neuroscientists, and ethicists who have long warned that PVS is far less clear than it is often portrayed. In doing so, the author brings long-overdue attention to a classification that lacks clinical support and is highly subjective.
The diagnosis of PVS goes beyond description; it’s often determinative and can function as both a figurative and literal death sentence. Once a patient is labeled “vegetative,” insurance providers will almost immediately withdraw coverage for therapies, rehabilitation, and other forms of care that could support recovery. The assumption quickly becomes that improvement is impossible, and, therefore, treatment is unnecessary. At that stage, families must either admit their loved one to a nursing home or bring them home, if they can provide the necessary care.
However, even more troubling, the diagnosis can also become a pathway to death. Because PVS is widely regarded as a condition devoid of awareness or meaningful life, it is often used to justify denying or withdrawing basic care, including food and water. In these cases, the PVS label itself becomes the reason for life-ending decisions, which are not made on certainty but on probabilities and subjective interpretations.
This is why Engelhart’s reporting carries such weight. Her article raises serious questions: How accurate are these diagnoses? How many patients have been misclassified? And how many lives have been prematurely ended based on assumptions that evolving science is now challenging?
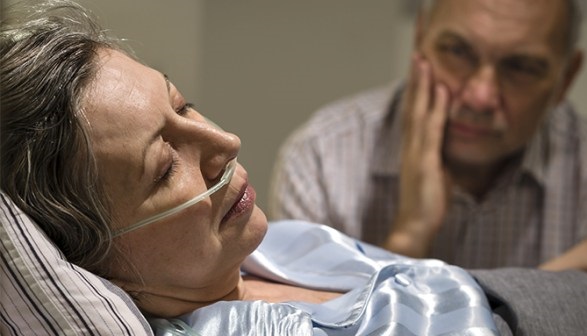
These are not hypothetical concerns. They are painfully real, as my family knows from the case of my sister, Terri Schiavo. For years, Terri was diagnosed as being in a persistent vegetative state. Based largely on such a diagnosis, a court ordered the withdrawal of her feeding tube, leading to her brutal death by dehydration and starvation over nearly two weeks. At the time, despite my family’s objections and testimony from multiple doctors on record with the court, the certainty of her diagnosis was widely accepted and rarely questioned by mainstream media.
Yet, the very questions Engelhart now highlights – about awareness, misdiagnosis rates, and the limits of clinical observation – strike at the heart of Terri’s case. If patients diagnosed as “vegetative” may, in fact, have some level of consciousness, then decisions like Terri’s, made under the notion of total unawareness, must be reexamined. This issue raises the very uncomfortable possibility that my sister, and others like her, may not have been as irreversibly unaware as doctors claimed.
This is where Engelhart’s article becomes more complicated. She references Terri’s autopsy, noting that her brain weighed significantly less than that of a typical adult.
Presented on its own, this detail appears to reinforce the ongoing narrative that Terri’s condition was beyond dispute. However, medical professionals have acknowledged that the human brain is approximately 75% water, so prolonged dehydration, such as the nearly two weeks Terri endured without food or water, can substantially reduce brain weight. Without this critical context, the autopsy reference is misleading.
This much is certain: continued reliance on the PVS diagnosis as a basis for life-ending decisions is deeply problematic. It places undue emphasis on a classification with highly questionable veracity. It also creates a system in which defenseless individuals may be denied both the chance to recover and, ultimately, the right to live, based on conclusions that may later prove incorrect.
At the same time, the article does important work by elevating awareness about brain injury and the challenges faced by patients and their families. It also highlights the advocacy of the organization my family started in response to my sister’s death: the Terri Schiavo Life & Hope Network, which continues to fight for better care, more accurate diagnoses, and the protection of medically defenseless individuals.
Engelhart’s piece starts an important public conversation that must lead to real change, not just acknowledge uncertainty. This includes expanding access to advanced diagnostic tools, ensuring rehabilitation is not prematurely denied, and – most importantly – following the updated guidelines from organizations such as the American Academy of Neurology, which recommends giving the brain adequate time and appropriate therapy to maximize the chance of recovery.
Above all, we must stop using a deeply flawed and immoral diagnosis as justification to end human lives, violating our God-given human dignity. In the end, the question is not just whether we are getting the science right. It is whether we are willing to confront what it means if we haven’t.
LifeNews Note: Bobby Schindler and his family work as patient advocates, establishing the non-profit Terri Schiavo Life & Hope Network in honor of his sister, Terri. Click here to learn more about the Life & Hope Network.








![Hegseth Demands Fitness Requirements, Says 'Fat Troops' 'Not Who We Are' [WATCH]](https://teamredvictory.com/wp-content/uploads/2025/09/Hegseth-Demands-Fitness-Requirements-Says-Fat-Troops-Not-Who-We-350x250.jpg)
